Back
PAD: Other
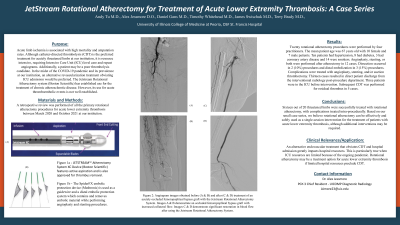
140 - JetStream Rotational Atherectomy for Treatment of Acute Lower Extremity Thrombosis: A Case Series

Alex Jessmore, D.O. – Resident Physician, University of Illinois College of Medicine at Peoria - OSF Healthcare; Timothy Whitehead, M.D. – Attending Physician, University of Illinois College of Medicine at Peoria - OSF Healthcare; James Swischuk, M.D. – Attending Physician, University of Illinois College of Medicine at Peoria - OSF Healthcare; Terry Brady, M.D. – Attending Physician, University of Illinois College of Medicine at Peoria - OSF Healthcare; Daniel Gans, M.D. – Attending Physician, University of Illinois College of Medicine at Peoria - OSF Healthcare
Purpose: Acute limb ischemia is associated with high mortality and amputation rates. While catheter-directed thrombolysis is the preferred treatment for acutely threatened limbs at our institution, it is resource intensive; requiring ICU level care and repeat angiograms. Additionally, a patient may be a poor thrombolysis candidate. In the midst of the COVID-19 pandemic and its prevalence at our institution, an alternative revascularization treatment obviating ICU admission would be preferred. The Jetstream Rotational Atherectomy system (Boston Scientific, Marlborough, Massachusetts) has established use for treatment of chronic atherosclerotic disease. However, its use for acute thromboembolic events is not well established.
Material and Methods: A retrospective review was performed of all the primary rotational atherectomy procedures performed for acute lower extremity thrombosis between March 2020 and October 2021 at our institution.
Results: Twenty rotational atherectomy procedures were performed by 4 practitioners. Mean age was 67 years with 10 female and 7 male patients. Ten were hypertensive, 8 were diabetic, 3 had coronary artery disease, and 14 were smokers. Angioplasty, stenting, or both were performed after atherectomy in 12 cases. Dissection occurred in 2 (10%) procedures and distal embolization in 3 (15%). Complications were treated with angioplasty, stenting, and/or suction thrombectomy. Thirteen cases resulted in direct patient discharge from the IR department. Three patients were in the ICU prior to intervention. Subsequent catheter-directed thrombolysis was performed for residual thrombus in 5 cases.
Conclusions: Sixteen out of 20 threatened limbs were successfully treated with rotational atherectomy, with complications treated intra-procedurally. Based on our small case series, we believe rotational atherectomy can be effectively and safely used as a single session intervention for the treatment of acute lower extremity thrombosis, although additional interventions may be required.
An alternative endovascular treatment that obviates catheter-directed thrombolysis and hospital admission greatly impacts hospital resources. This is particularly true when intensive care unit resources are limited due to the ongoing pandemic. Rotational atherectomy may be a treatment option for acute lower extremity thrombosis if limited hospital resources preclude catheter-directed thrombolysis.
Material and Methods: A retrospective review was performed of all the primary rotational atherectomy procedures performed for acute lower extremity thrombosis between March 2020 and October 2021 at our institution.
Results: Twenty rotational atherectomy procedures were performed by 4 practitioners. Mean age was 67 years with 10 female and 7 male patients. Ten were hypertensive, 8 were diabetic, 3 had coronary artery disease, and 14 were smokers. Angioplasty, stenting, or both were performed after atherectomy in 12 cases. Dissection occurred in 2 (10%) procedures and distal embolization in 3 (15%). Complications were treated with angioplasty, stenting, and/or suction thrombectomy. Thirteen cases resulted in direct patient discharge from the IR department. Three patients were in the ICU prior to intervention. Subsequent catheter-directed thrombolysis was performed for residual thrombus in 5 cases.
Conclusions: Sixteen out of 20 threatened limbs were successfully treated with rotational atherectomy, with complications treated intra-procedurally. Based on our small case series, we believe rotational atherectomy can be effectively and safely used as a single session intervention for the treatment of acute lower extremity thrombosis, although additional interventions may be required.
An alternative endovascular treatment that obviates catheter-directed thrombolysis and hospital admission greatly impacts hospital resources. This is particularly true when intensive care unit resources are limited due to the ongoing pandemic. Rotational atherectomy may be a treatment option for acute lower extremity thrombosis if limited hospital resources preclude catheter-directed thrombolysis.
