Back
Access and Closure
129 - Inguinal Ligament Safe Space Fallacy

Weston Andrews, MD – Resident, Vascular Surgery, University of Florida College of Medicine - Jacksonville; Rennette Zavala, MD – Resident, Vascular Surgery, University of Florida College of Medicine - Jacksonville; Edward Prange, MD – Resident, Vascular Surgery, University of Florida College of Medicine - Jacksonville; Erik Eadie, MD – Resident, Interventional Radiology, University of Florida College of Medicine - Jacksonville; Chase Parsons, MD – Resident, Interventional Radiology, University of Florida College of Medicine - Jacksonville; Derrick Tran, MD – Resident, Interventional Radiology, University of Florida College of Medicine - Jacksonville; Miguel Villalobos, MD – Assistant Professor, Vascular Surgery, University of Florida College of Medicine - Jacksonville; Henry Veldenz, MD – Associate Professor, Vascular Surgery, University of Florida College of Medicine - Jacksonville
Purpose: To investigate factors contributing to retroperitoneal hemorrhage after femoral access.
Material and Methods: Nuance mPower search for reports from CT studies containing the keywords retroperitoneal hemorrhage/hematoma and femoral pseudoaneurysm/extravasation followed by chart review. Inclusion criteria were presence of retroperitoneal hemorrhage, and pseudoaneurysm at a recent arterial access site. Exclusion criterion was etiology of retroperitoneal hemorrhage other than iatrogenic from arterial access.
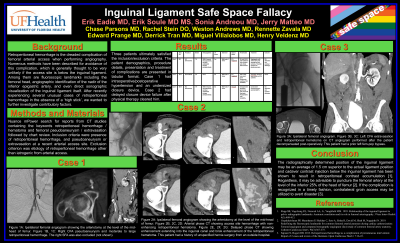
Results: 34 patients were initially identified, with only 6 meeting inclusion criteria; 4/6 had alternative etiology of retroperitoneal hemorrhage and were excluded. Ultrasound was used for access and ultimately upsizing to a 7 Fr sheath in both patients and both access sites were below the inguinal ligament. Patient 1 was a 63-year-old male with RLE tissue loss (heel ulcer) in the setting of bilateral long-segment SFA occlusions status post failed L femoral-popliteal bypass and amputation of LLE digits 1-4 undergoing R SFA revascularization. Directional atherectomy and DCB angioplasty was performed to the R SFA, restoring patency. The patient received 9000 U heparin and the groin was closed with a Vascade device. The complications presented with intraoperative L flank pain/groin lump and post-operative hypotension. Patient 2 was a 65-year-old female with claudication from bilateral multifocal SFA stenoses and a short segment proximal L SFA occlusion. Directional atherectomy and DCB angioplasty was performed to the L SFA, restoring patency. The patient received 5000 U heparin and the groin was closed with a 6 Fr AngioSeal device after the pre-closure R femoral angiogram demonstrated no evidence of pseudoaneurysm/hemorrhage. The complications presented when she returned to the ED after two days with RLE rest pain and the R CFA was found to be occluded.
Conclusions: Concomitant access site pseudoaneurysm and retroperitoneal hemorrhage in patient 1 was attributed to prior groin surgery allowing communication to the retroperitoneum from below the inguinal ligament. A false sense of security regarding accessing the CFA inferior to the inguinal ligament and foregoing ipsilateral femoral angiography prior to closure may have delayed recognition of the potentially treatable complication. Concomitant access site pseudoaneurysm, retroperitoneal hemorrhage, and ipsilateral CFA occlusion in patient 2 was attributed to intraprocedural/postprocedural hypertension and undersizing of the closure device.
Material and Methods: Nuance mPower search for reports from CT studies containing the keywords retroperitoneal hemorrhage/hematoma and femoral pseudoaneurysm/extravasation followed by chart review. Inclusion criteria were presence of retroperitoneal hemorrhage, and pseudoaneurysm at a recent arterial access site. Exclusion criterion was etiology of retroperitoneal hemorrhage other than iatrogenic from arterial access.
Results: 34 patients were initially identified, with only 6 meeting inclusion criteria; 4/6 had alternative etiology of retroperitoneal hemorrhage and were excluded. Ultrasound was used for access and ultimately upsizing to a 7 Fr sheath in both patients and both access sites were below the inguinal ligament. Patient 1 was a 63-year-old male with RLE tissue loss (heel ulcer) in the setting of bilateral long-segment SFA occlusions status post failed L femoral-popliteal bypass and amputation of LLE digits 1-4 undergoing R SFA revascularization. Directional atherectomy and DCB angioplasty was performed to the R SFA, restoring patency. The patient received 9000 U heparin and the groin was closed with a Vascade device. The complications presented with intraoperative L flank pain/groin lump and post-operative hypotension. Patient 2 was a 65-year-old female with claudication from bilateral multifocal SFA stenoses and a short segment proximal L SFA occlusion. Directional atherectomy and DCB angioplasty was performed to the L SFA, restoring patency. The patient received 5000 U heparin and the groin was closed with a 6 Fr AngioSeal device after the pre-closure R femoral angiogram demonstrated no evidence of pseudoaneurysm/hemorrhage. The complications presented when she returned to the ED after two days with RLE rest pain and the R CFA was found to be occluded.
Conclusions: Concomitant access site pseudoaneurysm and retroperitoneal hemorrhage in patient 1 was attributed to prior groin surgery allowing communication to the retroperitoneum from below the inguinal ligament. A false sense of security regarding accessing the CFA inferior to the inguinal ligament and foregoing ipsilateral femoral angiography prior to closure may have delayed recognition of the potentially treatable complication. Concomitant access site pseudoaneurysm, retroperitoneal hemorrhage, and ipsilateral CFA occlusion in patient 2 was attributed to intraprocedural/postprocedural hypertension and undersizing of the closure device.
