Back
Introduction: Checkpoint inhibitor therapy has improved outcomes for patients with bladder cancer, however not all patients achieve clinical response. Biomarkers such as PDL1 tumor expression and high tumor mutational burden (TMB) have been associated with improved response rates. We utilized the Tempus Lens platform, a web-based library of clinical and molecular data, to determine if TMB, PDL1 expression, or somatic tumor alterations were associated with response to immunotherapy.
Methods: Using the Lens platform managed by Tempus (Chicago, Illinois), we selected patients with stage 3 and 4 bladder cancer who received PD1/PDL1 checkpoint inhibitor therapy. Somatic gene mutations via next-generation sequencing (NGS), TMB (> 10 mutations/Mb), and PDL1 expression on tumor and immune cells were assessed against rates of disease response. Analyses were performed with chi-square test at significance of p = 0.05.
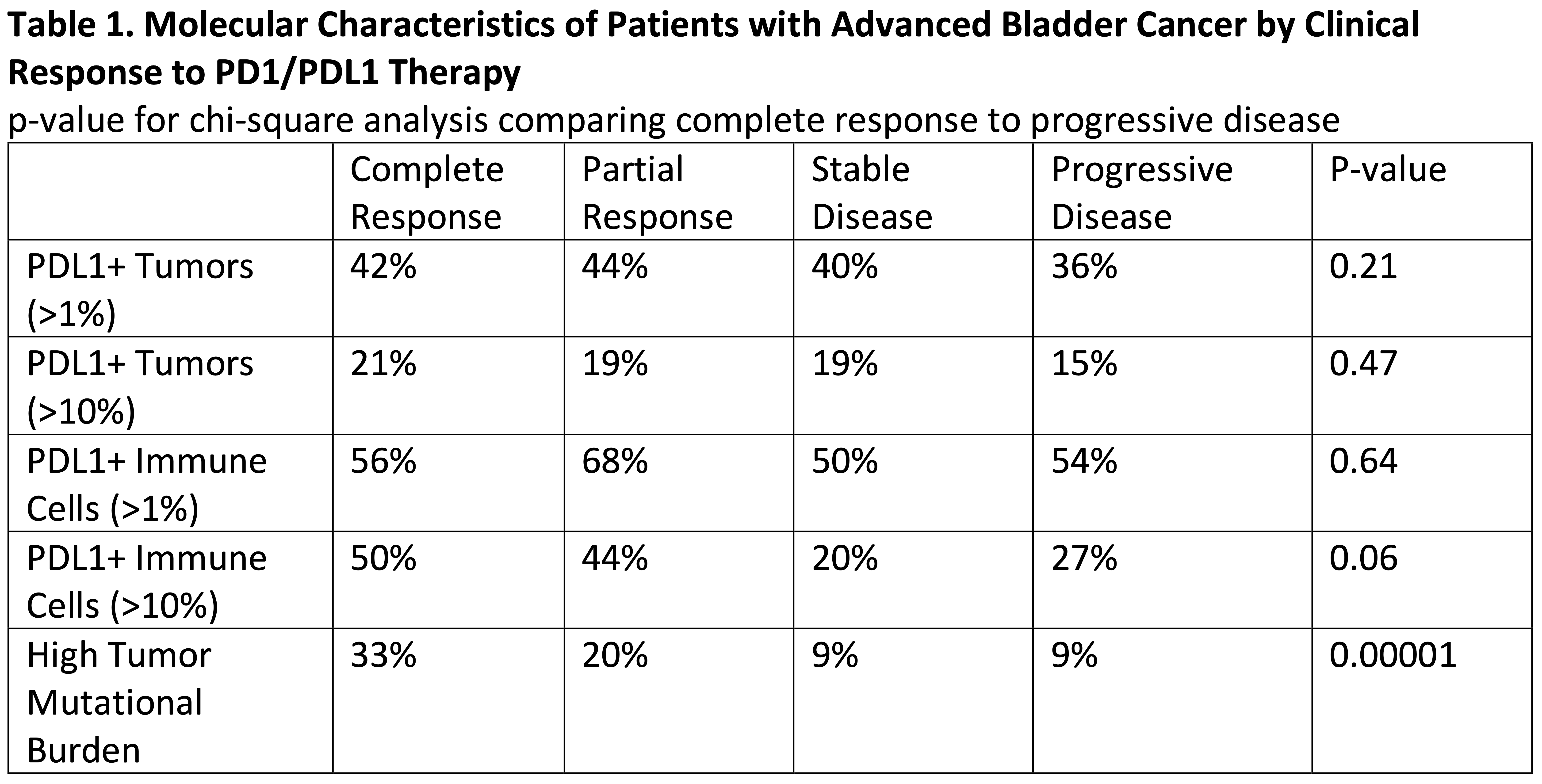
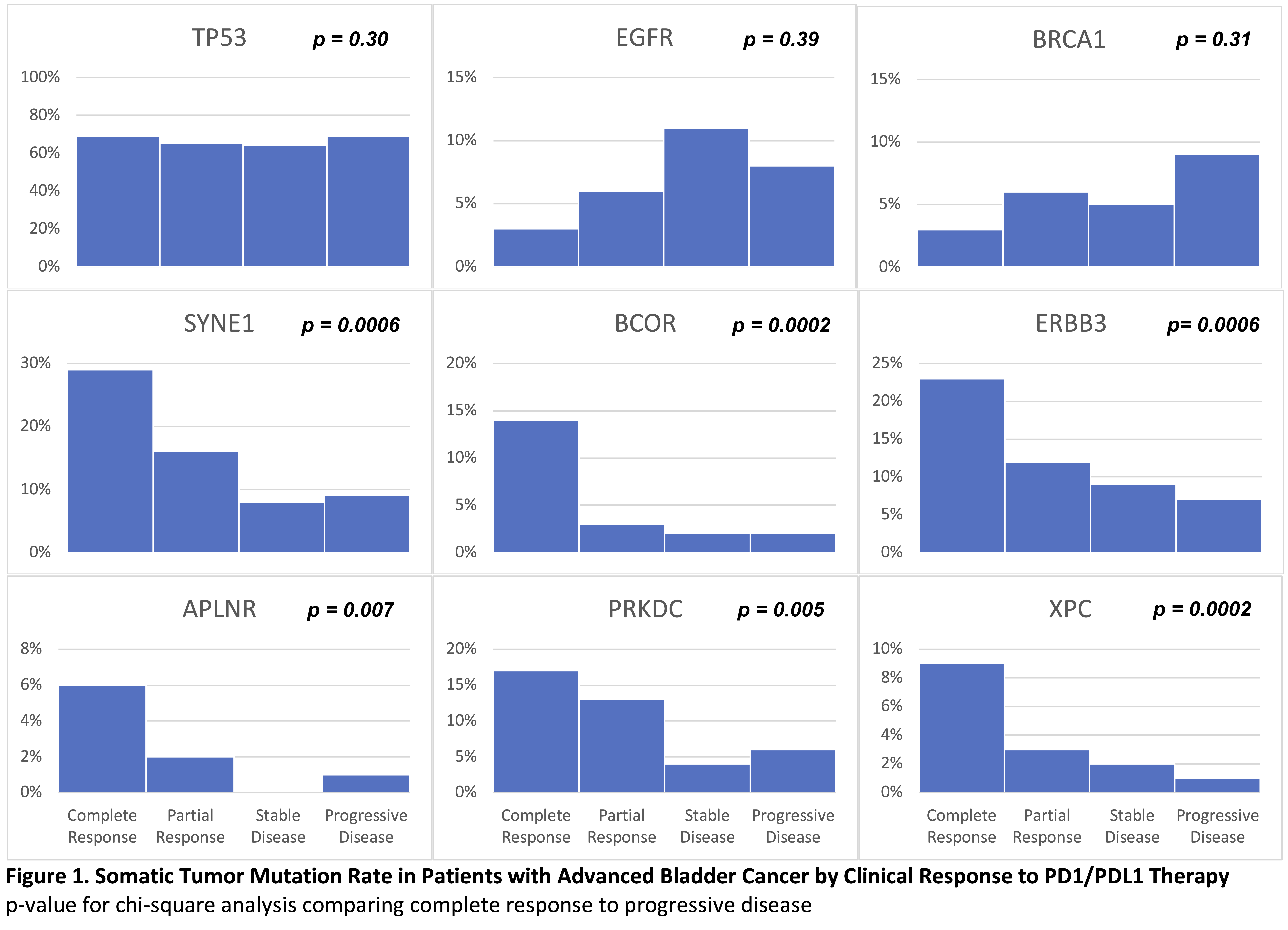
Results: 5.4 million patients were assessed as part of the Lens platform. 4,041 patients with stage 3 or 4 bladder cancer were identified. Clinical response to PD1/PDL1 therapy and NGS data was available for 442. In this dataset PDL1 tumor expression was not associated with improved treatment response, however PDL1 expression on greater than 10% of tumor infiltrating immune cells was more closely linked, as this was seen in 50% of patients with complete response compared to 27% with progressive disease (p = 0.06) (Table 1). In addition, certain somatic alterations were associated with complete response while others were associated with progressive disease (Figure 1). As previously described, patients with complete response were more likely to have high TMB than those with progressive disease (p < 0.0001).
Conclusions: While PDL1 tumor expression is thought to be predictive of immunotherapy response rates, our data suggest that immune infiltrate PDL1 expression may be a better predictor. In addition, certain somatic alterations may predict response or lack of response to immunotherapy. SOURCE OF
Funding: none
Moderated Poster Session
Session: MP32: Bladder Cancer: Invasive II
MP32-13: PDL1 Expression on Tumor Infiltrating Immune Cells and Somatic Gene Alterations Associated with Response to Immunotherapy in Patients with Advanced Bladder Cancer
Saturday, April 29, 2023
9:30 AM – 11:30 AM CST
Location: S403
- JH
John R. Heard, MD, MS (he/him/his)
Resident Physican
Cedars-Sinai Medical Center
Poster Presenter(s)
Introduction: Checkpoint inhibitor therapy has improved outcomes for patients with bladder cancer, however not all patients achieve clinical response. Biomarkers such as PDL1 tumor expression and high tumor mutational burden (TMB) have been associated with improved response rates. We utilized the Tempus Lens platform, a web-based library of clinical and molecular data, to determine if TMB, PDL1 expression, or somatic tumor alterations were associated with response to immunotherapy.
Methods: Using the Lens platform managed by Tempus (Chicago, Illinois), we selected patients with stage 3 and 4 bladder cancer who received PD1/PDL1 checkpoint inhibitor therapy. Somatic gene mutations via next-generation sequencing (NGS), TMB (> 10 mutations/Mb), and PDL1 expression on tumor and immune cells were assessed against rates of disease response. Analyses were performed with chi-square test at significance of p = 0.05.
Results: 5.4 million patients were assessed as part of the Lens platform. 4,041 patients with stage 3 or 4 bladder cancer were identified. Clinical response to PD1/PDL1 therapy and NGS data was available for 442. In this dataset PDL1 tumor expression was not associated with improved treatment response, however PDL1 expression on greater than 10% of tumor infiltrating immune cells was more closely linked, as this was seen in 50% of patients with complete response compared to 27% with progressive disease (p = 0.06) (Table 1). In addition, certain somatic alterations were associated with complete response while others were associated with progressive disease (Figure 1). As previously described, patients with complete response were more likely to have high TMB than those with progressive disease (p < 0.0001).
Conclusions: While PDL1 tumor expression is thought to be predictive of immunotherapy response rates, our data suggest that immune infiltrate PDL1 expression may be a better predictor. In addition, certain somatic alterations may predict response or lack of response to immunotherapy. SOURCE OF
Funding: none


