Laboratory Research
(LR-024) A Human Keratin Hydrogel Matrix Modulates Cytokine Production in Keratinocytes and Fibroblasts In Vitro
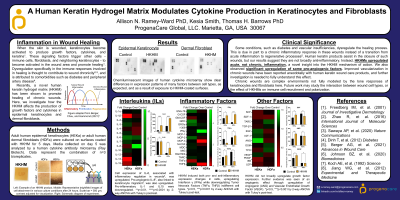
The wound healing process requires a dynamic inflammatory environment, beginning with a spike in pro-inflammatory factors followed by pro-regenerative molecules that drive wound closure while reducing inflammation. Non-healing wounds are shown to lack these dynamics, instead having chronic, low-level expression of pro-inflammatory factors. This suggests combining pro- and anti-inflammatory effects may benefit healing in these wounds. It is currently unknown how the human keratin hydrogel matrix (HKHM), a novel wound dressing, affects the wound inflammatory environment. This work investigates how HKHMs alter cytokine expression in keratinocytes and dermal fibroblasts in vitro to better understand their effect on chronic wounds.
Methods: Either human keratinocytes or adult human dermal fibroblasts (HDFa’s) were plated at equal densities on tissue culture plastic (control) or HKHM-coated culture surfaces, and grown for 5 days with cell media changed every other day. After 5 days, cell media from each group was incubated on a semiquantitative, sandwich-based chemiluminescent antibody microarray detecting 42 different human cytokines according to the manufacturer’s protocol. The resultant chemiluminescence was quantified using a CCD camera, and fold change in expression was calculated between HKHM and control surfaces.
Results:
Distinct expression patterns were observed between keratinocytes and fibroblasts, with an overall trend of cytokine downregulation in both cell types. However, there was a combination of up- and downregulation of some pro-inflammatory factors in both. Inflammatory cytokines Tumor Necrosis Factor alpha (TNFa) and Interferon-gamma (IFNg) were downregulated in both cell types, as were the chemoattractant proteins GRO and GRO-alpha, but Interleukin-6 was upregulated. Human keratinocytes cultured on HKHM specifically upregulated Insulin-Like Growth Factor 1 (IGF-1), Interleukin-15, and Stromal-Derived Factor 1 (SDF-1). However, HDFa’s showed more upregulation of Interleukin-8 and Colony Stimulating Factor 3 (G-CSF).
Discussion:
Recent research has shown that a lack of dynamic inflammatory response is associated with wound chronicity, particularly in elderly and diabetic patients. Analysis of cytokine expression in two skin cell types, keratinocytes and dermal fibroblasts, suggests that HKHM does not promote a specific pro- or anti-inflammatory phenotype, but rather modulates expression of cytokines that have been demonstrated to promote a more normal wound inflammatory response. To better understand this response, future work will study how the inflammatory environment in a chronic wound responds to HKHM in vivo, where these cell types can interact and respond to the differential expression profiles.
Trademarked Items:
References:

.png)