Back
Clinical Research
(CR-021) Evaluating Outcomes in Chronically Anticoagulated Patients Receiving Split-Thickness Skin Grafting for Diabetic Foot Ulcers

Co-Author(s):
Elliot Walters, MD – Department of Surgery – University of Texas Medical Branch at Galveston; Alen Palackic, MD – Department of Surgery – University of Texas Medical Branch at Galveston; Camila Franco Mesa, MD – PGY-1, Department of Surgery, University of Texas Medical Branch at Galveston; Steven Wolf, MD – Professor and Chief, Division of Burn and Trauma Surgery, University of Texas Medical Branch at Galveston
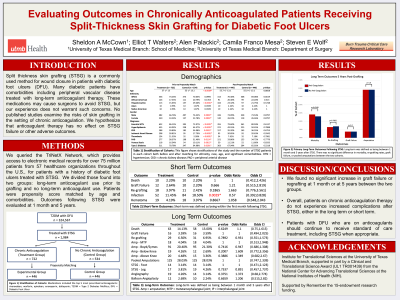
<b>Introduction</b>: <strong id="docs-internal-guid-2194b991-7fff-7f78-ca96-9c4db366f256" style="font-weight: normal;"><span style="font-size: 11pt; font-family: 'Times New Roman'; color: #000000; background-color: transparent; font-weight: 400; font-style: normal; font-variant: normal; text-decoration: none; vertical-align: baseline; white-space: pre-wrap;">Split thickness skin grafting (STSG) is a common method for wound closure in patients with diabetic foot ulcers. In some cases, diabetic patients present with co-morbidities that require long-term anticoagulation therapy, especially after receiving interventions for peripheral artery disease. The use of anticoagulants, specifically, the complications associated with them, can be discouraging to surgeons when considering STSG. However, the current literature available describing the risk of skin grafting in the setting of chronic anticoagulation is extremely limited. The goal of the following study is to evaluate outcomes of STSG in the setting of chronic anticoagulation across a large multicenter database.</span></strong><br/><br/><b>Methods</b>: <strong id="docs-internal-guid-668275c2-7fff-42f2-e489-5cc414635df0" style="font-weight: normal;"><span style="font-size: 11pt; font-family: 'Times New Roman'; color: #000000; background-color: transparent; font-weight: 400; font-style: normal; font-variant: normal; text-decoration: none; vertical-align: baseline; white-space: pre-wrap;">We queried the TriNetX Network, which provides access to electronic medical records for over 75 million patients from 57 healthcare organizations throughout the U.S., for patients with a history of diabetic foot ulcers treated with STSG. We divided those found into two groups: long-term anticoagulant use prior to grafting and no long-term anticoagulant use. Patients were propensity score matched by age, ethnicity, essential hypertension, hyperlipidemia, diabetes, ischemic heart disease, chronic kidney disease, venous insufficiency, pulmonary embolism, and peripheral vascular disease. Outcomes following STSG were evaluated at 1 month and 5 years post procedure. </span></strong><br/><br/><b>Results</b>: <strong id="docs-internal-guid-0f51a678-7fff-8c1e-1389-e5618e6e7fd7" style="font-weight: normal;"><span style="font-size: 11pt; font-family: 'Times New Roman'; color: #000000; background-color: transparent; font-weight: 400; font-style: normal; font-variant: normal; text-decoration: none; vertical-align: baseline; white-space: pre-wrap;">We identified 324,567 diabetic patients with foot ulcers, 1,984 patients were treated with STSG. We identified 722 patients with prior anticoagulation; 446 of these patients were matched to 446 patients with no prior anticoagulation. At 1 month post-STSG, the anticoagulated group showed no significant increase in death (p = 1.0), graft failure (p = 0.666), or regrafting (p = 0.1865). At 5 years, we found no significant increase in mortality (p = 0.6249), graft failure (p = 1.0), regrafting (p = 0.7892), or rates of lower extremity amputation at any level (p = 1.0). </span></strong><br/><br/><b>Discussion</b>: <p dir="ltr" style="line-height: 1.2839972727272726; margin-top: 6pt; margin-bottom: 12pt;"><span style="font-size: 11pt; font-family: 'Times New Roman'; color: #000000; background-color: transparent; font-weight: 400; font-style: normal; font-variant: normal; text-decoration: none; vertical-align: baseline; white-space: pre-wrap;">Anticoagulation therapy does not lead to increased short-term post-operative complications such as graft failure, re-grafting, or increased amputation rates after STSG for wound closure. Furthermore, long-term complications and disease progression remain low for this group as well. Short-term and long-term outcomes of STSG in the chronically anticoagulated patient with diabetic foot ulcers are well within acceptable ranges and grafting should be performed without hesitation. </span></p><br/><br/><b>Trademarked Items</b>: <br/><br/><b>References</b>: <br/><br/>

.png)
