Practice Innovations
(PI-023) Assessing Lower Extremity Hypoperfusion in ICU Patients on Vasopressors Using Infrared Thermography
Vasopressors are commonly used in critically ill patients to increase mean arterial pressure (MAP) by constricting distal blood vessels1. Distal hypoperfusion related to vasopressor use is associated with ischemic injury to the extremities, which can lead to tissue necrosis, wounding, and may ultimately require amputation2,3. Infrared thermography is a reliable tool to identify changes in tissue perfusion, allowing clinicians to identify areas of regional temperature change indicative of distal hypoperfusion4,5,6. Enhanced skin assessment using infrared thermography in critically ill patients is aligned with current best practice recommendations and improves understanding of primary etiology of skin changes. The purpose of this study is to compare distal lower extremity hypoperfusion in critical care patients who were treated with and without vasopressors using infrared thermography scanning.
Methods:
A retrospective analysis was conducted using a convenience sample of patients admitted to two ICUs at a 900 bed level-1 trauma center. Thermography was used to evaluate temperature change of lower extremities in patients with and without vasopressors. Nurses received standardized education on proper scanning technique and were instructed to scan all patients within 8 hours of admission. A blinded analysis of thermographic images was performed by the Wound Care Team. Temperature change was determined by assessing knee to heel temperature differential using infrared thermography.
Results:
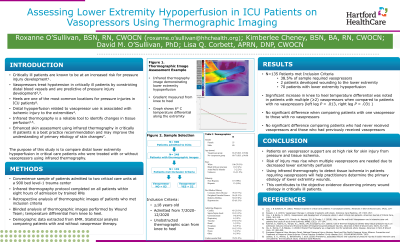
One hundred and fifty patients met inclusion criteria. Of those, seventy (70) demonstrated regional temperature changes associated with hypoperfusion. Significant knee to heel temperature differential was noted in patients with multiple (≥2) vasopressors infusing at the time of imaging, when compared to patients with no vasopressors (left leg P = .013, right leg P = .031). No significance was found when comparing patients with only one vasopressor and those with no vasopressors. Additional analysis was performed on the following variables: primary diagnosis, comorbidities, sex, race, anticoagulant, and pressure injury outcomes.
Discussion:
Patients requiring vasopressor support to maintain hemodynamic stability are at high risk for skin injury. Risk of injury may increase when multiple vasopressors are needed as distal lower extremity hypoperfusion increases. This will contribute to the evidence discerning primary wound etiology in critically ill patients.
Trademarked Items:
References: 1. Russell, J. A. (2019). Vasopressor therapy in critically ill patients with shock. Intensive Care Medicine, 45: 1503-1517. https://link.springer.com/article/10.1007/s00134-019-05801-z Last accessed 3/9/21
2. Cox, J. & Schallom, M. (2021) Pressure injuries in critical care patients: A conceptual schema. Advances in Skin & Wound Care, 34(3), 124-131. https://journals.lww.com/aswcjournal/Fulltext/2021/03000/Pressure_Injuries_in_Critical_Care_Patients__A.4.aspx?context=LatestArticles
3. Newbury, A., Harper, K.D., Trionfo, A., Ramsey, F.V., & Thoder, J.J. (2018). Why not life and limb? Vasopressor use in intensive care unit patients the cause of acute limb ischemia. HAND, 15(2): 177-184. https://doi.org/10.1177%2F1558944718791189 Last accessed 3/30/21
4. Tattersall, G.J. (2016). Infrared Thermography: A non-invasive window into thermal physiology. Comparative Biochemistry and Physiology, 202: 78-98. https://doi.org/10.1016/j.cbpa.2016.02.022
5. Ilo, A., Romsi, P., & Makela, J. (2020) Infrared Thermography as a diagnostic tool for peripheral artery disease. Advances in Skin & Wound Care, 33: 482-8. doi:10.109/01.ASW.0000694156.62834.8b
6. Chang, W., Wang, C., Cheng, Y., Hung, Y., Lin, T., Chen, W., Su, C., Hsu, C., Liu, T., & Lee, W. (2020). Plantar thermography predicts freedom from major amputation after endovascular therapy in critical limb ischemic patients. Medicine, 99(46): e22391. https://dx.doi.org/10.1097/MD.0000000000022391

.png)
