Case Series/Study
(CS-123) Fish Skin Graft* (FSG) for the treatment of hard-to-heal venous leg ulcers (VLU)
Venous leg ulcers (VLU) are non-healing full-thickness skin defects resultant from chronic venous diseases, including venous hypertension, a consequence of valve reflux often accompanied by venous obstruction. VLUs impact approximately three out of ten Americans, and treatment costs the U.S. an estimated 2.5 million dollars annually1. The complex pathophysiology associated with VLUs makes treatment challenging. The clinical manifestation of ulceration is a significant burden on the patient, often causing edema, pain, limb heaviness, and poor ambulation1. Advanced skin biologics have implications for expediting healing, thus improving quality of life and patient care. A relatively new and novel biologic, Fish skin graft (FSG) has been used and proven to be a highly effective adjunctive therapy for treating VLUs2.
Methods:
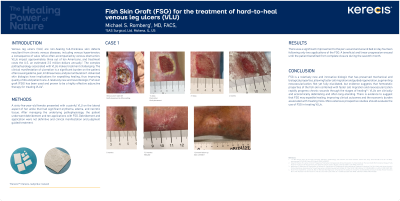
A sixty-five-year-old female presented with a painful VLU on the lateral aspect of her ankle that had significant erythema, edema, and necrotic tissue. After managing the underlying pathophysiology, the patient underwent debridement and ten applications with FSG. Debridement and application were not definitive and clinical manifestation and judgment guided treatment.
Results:
There was a significant improvement to the peri-wound and wound bed on day fourteen following only two applications of the FSG. A beneficial and linear progression ensued until the patient benefited from complete closure during the seventh month.
Discussion:
FSG is a relatively new and innovative biologic that has preserved mechanical and biological properties, allowing faster cell migration and guided regeneration, augmenting neovascularization. Not yet fully elucidated, but evidence suggests that hemostatic properties of the fish skin combined with faster cell migration and neovascularization rapidly progress chronic wounds through the stages of healing3,4. VLUs are clinically and economically debilitating and often long-standing. There is evidence to suggest that FSG may expedite healing, improving clinical outcomes and the economic burden associated with treating VLUs. More extensive prospective studies should evaluate the use of FSG in treating VLUs.
Trademarked Items: *KerecisTM, Kerecis, Isafjordur, Iceland
References: 1. Lal BK. Venous ulcers of the lower extremity: Definition, epidemiology, and economic and social burdens. Semin Vasc Surg. 2015 Mar;28(1):3-5. doi: 10.1053/j.semvascsurg.2015.05.002. Epub 2015 May 8. PMID: 26358303.
2. Yang CK, Polanco TO, Lantis JC 2nd. A Prospective, Postmarket, Compassionate Clinical Evaluation of a Novel Acellular Fish-skin Graft Which Contains Omega-3 Fatty Acids for the Closure of Hard-to-heal Lower Extremity Chronic Ulcers. Wounds. 2016 Apr;28(4):112-8. PMID: 27071138.
3. Magnusson S, Baldursson BT, Kjartansson H, Rolfsson O, Sigurjonsson GF. Regenerative and Antibacterial Properties of Acellular Fish Skin Grafts and Human Amnion/Chorion Membrane: Implications for Tissue Preservation in Combat Casualty Care. Mil Med. 2017 Mar;182(S1):383-388. doi: 10.7205/MILMED-D-16-00142. PMID: 28291503.
4. Stone R 2nd, Saathoff EC, Larson DA, Wall JT, Wienandt NA, Magnusson S, Kjartansson H, Natesan S, Christy RJ. Accelerated Wound Closure of Deep Partial Thickness Burns with Acellular Fish Skin Graft. Int J Mol Sci. 2021 Feb 4;22(4):1590. doi: 10.3390/ijms22041590. PMID: 33557424; PMCID: PMC7915828.

.png)