Case Series/Study
(CS-113) A case study: Successful early autologous skin grafting after significant debridement of skin necrosis from IV Xylazine and Fentanyl abuse.
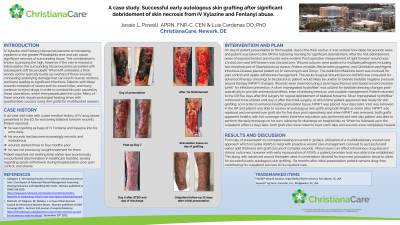
IV Xylazine and Fentanyl abuse has become an increasing epidemic in the greater Philadelphia area and can cause significant necrosis of surrounding tissue. This combination is known to prolong the high, however, if the vein is missed or extravasates, the surrounding tissue becomes ulcerated with subsequent soft tissue death. When left untreated, a thick woody eschar typically builds up overtop of these wounds, concealing underlying damage that can reach muscle, tendons, and bone leading to significant infections. Patients with these wounds complain of severe pain to wound sites, and many continue to inject drugs in order to combat this pain caused by these ulcerations, which perpetuates the cycle. Many of these wounds require prolonged healing times with questionable success using skin grafts for multifaceted reasons.
Methods:
A 40-year-old male with PMH of IV drug abuse presented to the ED for worsening bilateral forearm wounds. Patient reported he was injecting 24 bags of IV Fentanyl & Xylazine into his arms daily and that these wounds had become increasingly necrotic and malodorous. He reported these wounds started 3-4 months prior and he had not previously sought treatment for them. Due to the thick eschar, it was unclear how deep these wounds were, and patient was taken to the OR the following morning for significant debridement. After the first debridement, areas of exposed tendon and muscle were evident. Wound cultures were positive for multiple pathogens. Patient was placed on vancomycin and Zosyn. Addiction team was involved for pain control and opiate withdrawal management. Acute Surgical Wound Service (ASWS) was consulted for advanced therapy dressings to be placed as patient would likely be unable to tolerate bedside NPWT changes. A silver impregnated hydrofiber was used, and patient returned to the OR 5 days later for repeat debridement. NPWT was placed 6 days later. At next OR, VAC was removed and patient was grafted. Patient’s grafts looked healthy and he was able to perform the daily dressings on his own and was discharged on hospital day 21. When he followed up in the outpatient office 11 days later, both grafts were noted to have 100% take.
Results:
Discussion: From day of presentation to complete healing occurred in 32 days. Patient has been successful with outpatient drug rehab since hospitalization. Utilization of a multidisciplinary wound care approach which includes ASWS to help with proactive wound care management can lead to successful and earlier STSG closure of complex wounds.
Trademarked Items:
References:

.png)