Back
Poster, Podium & Video Sessions
Moderated Poster
MP14: Stone Disease: Surgical Therapy (including ESWL) I
MP14-03: Does the Position and Size of the Ureteral Access Sheath Affect Renal Pressures During Ureteroscopy? Intrarenal Pressure Measurement Using a Concept Single-Use Digital Flexible Ureteroscope
Friday, May 13, 2022
2:45 PM – 4:00 PM
Location: Room 225
Ben H. Chew*, Nabil Shalabi, K.F. Victor Wong, Roman Herout, Alina Reicherz, Vancouver, Canada, Naeem Bhojani, Montreal, Canada

Ben Chew, MD, MSC, FRCSC
Associate Professor of Urology
University of British Columbia
Poster Presenter(s)
Introduction: Ureteral access sheaths (UAS) facilitate ureteroscopy and one reported benefit is reduced intrarenal pressure. We sought to determine if the position of the UAS made a difference in renal pressure utilizing a concept pressure-sensing ureteroscope. We also sought to determine if different UAS sizes could impact renal pressure.
Methods: A concept single use digital flexible ureteroscope with pressure monitoring technology (Boston Scientific, USA, concept device/technology, not available for sale) was utilized in this study. Utilizing a live-anesthetized porcine model, pressure was verified by measuring pressure through a 5Fr ureteral catheter (via monitor HP78354A as a reference) compared to readings from the concept ureteroscope. Next, an anesthetized porcine model was tested with different sized ureteral access sheaths (UASs) (11/13, 12/14, and 13/15 Fr) in 3 different locations within the urinary system: 1. in the renal pelvis, 2. below the ureteropelvic junction and 3. in the distal ureter. A pressurized bag at 150mmHg was used to deliver irrigation. Pressure measurements were taken with each parameter using the concept ureteroscope after the renal collecting system had reached a steady state.
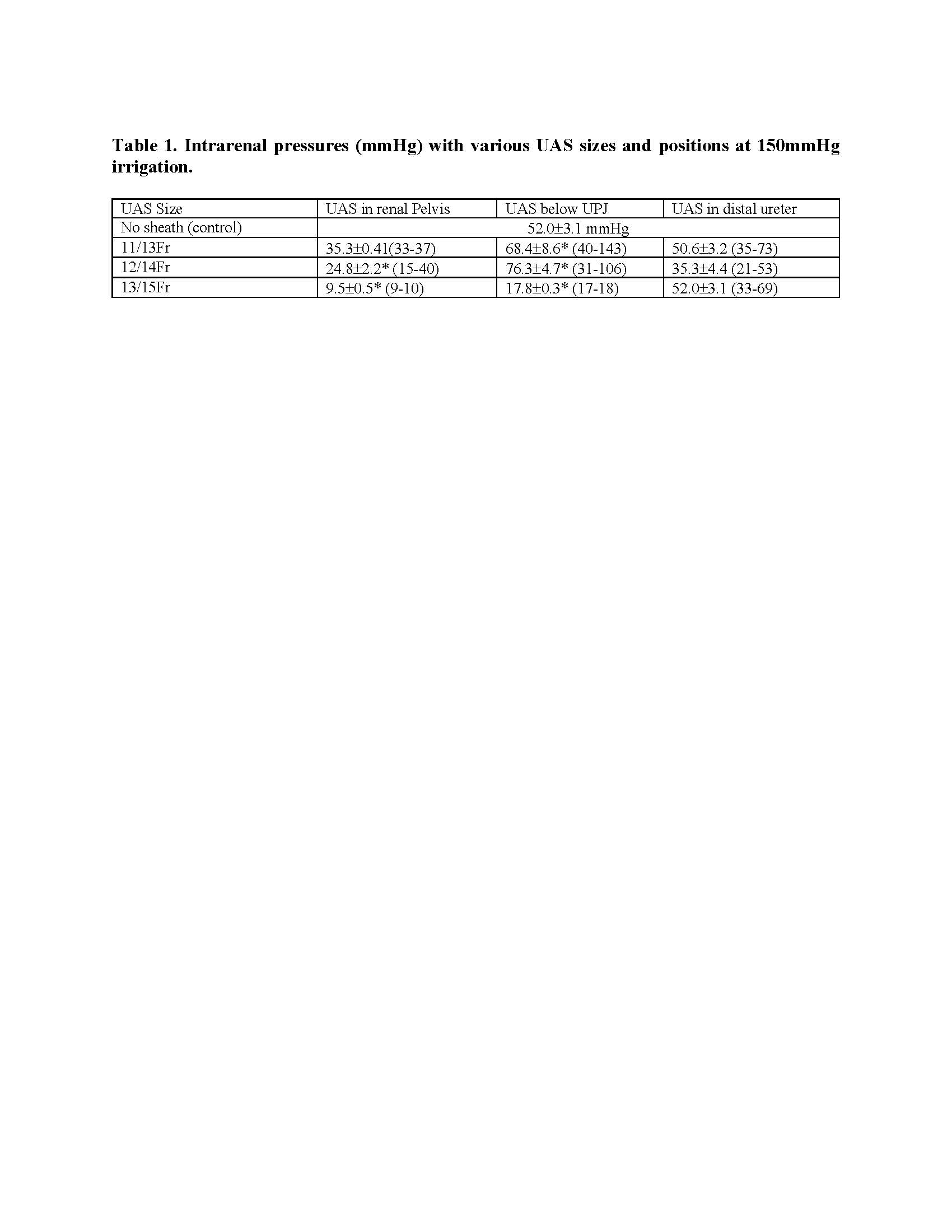
Results: Intra-renal pressure readings from the concept ureteroscope strongly corelated with the reference device (p=0.972). The lowest pressures occurred with the UAS in the renal pelvis for the 2 largest UAS sizes. If the UAS is below the UPJ, pressure significantly increased in the 11/13 and 12/14 UASs. Only the 13/15 reduced pressure when below the UPJ. None of the UASs in the distal ureter reduced pressure significantly from control. The 12/14 UAS in the renal pelvis had statistically lower pressure than control (p=0.001) and the 11/13 (p < 0.0001), but was not as low as the 13/15 (p=0.033).
Conclusions: Overall, the largest UAS (13/15Fr) offered the lowest pressure in most positions. . Placing the UAS in the distal ureter did not significantly reduce intrarenal pressure with any UAS. This data suggests to ideally use a >12/14Fr sized UAS in the renal pelvis to obtain the least pressure reduction during ureteroscopy. Further studies are needed to evaluate the clinical significance and sequelae of intra-renal pressure and to determine safe levels.
Source of Funding: This work was supported by Boston Scientific Inc.
Methods: A concept single use digital flexible ureteroscope with pressure monitoring technology (Boston Scientific, USA, concept device/technology, not available for sale) was utilized in this study. Utilizing a live-anesthetized porcine model, pressure was verified by measuring pressure through a 5Fr ureteral catheter (via monitor HP78354A as a reference) compared to readings from the concept ureteroscope. Next, an anesthetized porcine model was tested with different sized ureteral access sheaths (UASs) (11/13, 12/14, and 13/15 Fr) in 3 different locations within the urinary system: 1. in the renal pelvis, 2. below the ureteropelvic junction and 3. in the distal ureter. A pressurized bag at 150mmHg was used to deliver irrigation. Pressure measurements were taken with each parameter using the concept ureteroscope after the renal collecting system had reached a steady state.
Results: Intra-renal pressure readings from the concept ureteroscope strongly corelated with the reference device (p=0.972). The lowest pressures occurred with the UAS in the renal pelvis for the 2 largest UAS sizes. If the UAS is below the UPJ, pressure significantly increased in the 11/13 and 12/14 UASs. Only the 13/15 reduced pressure when below the UPJ. None of the UASs in the distal ureter reduced pressure significantly from control. The 12/14 UAS in the renal pelvis had statistically lower pressure than control (p=0.001) and the 11/13 (p < 0.0001), but was not as low as the 13/15 (p=0.033).
Conclusions: Overall, the largest UAS (13/15Fr) offered the lowest pressure in most positions. . Placing the UAS in the distal ureter did not significantly reduce intrarenal pressure with any UAS. This data suggests to ideally use a >12/14Fr sized UAS in the renal pelvis to obtain the least pressure reduction during ureteroscopy. Further studies are needed to evaluate the clinical significance and sequelae of intra-renal pressure and to determine safe levels.
Source of Funding: This work was supported by Boston Scientific Inc.


.jpg)
.jpg)