Back
Poster, Podium & Video Sessions
Best Poster Award
MP51: Prostate Cancer: Staging
MP51-17: Demographics and socioeconomic description of patients with prostate cancer in whom a prostate-specific membrane antigen PET was performed: a single-institution, retrospective analysis in NYC
Sunday, May 15, 2022
4:30 PM – 5:45 PM
Location: Room 222
juana martinez*, Kritika Subramanian, Muhammad Niaz, Ted Getz, Amie Patel, Joseph Osborne, Scott Tagawa, NY, NY
- JM
Poster Presenter(s)
Introduction: Prostate-specific membrane antigen (PSMA) PET imaging has improved detection rate of PC lesions, including in low serum PSA values, and has recently become commercially available. While some data exist that outcomes are similar across race/ethnicity in those participating in clinical trials, the advent of precision medicine and molecular imaging might lead to a worsening of inequities. We hypothesized that the demographic population which has access to this imaging modality may not be truly representative of the entire PC community.
Methods: Patients with PC who underwent a PSMA PET scan between January 2018 and October 2021, were extracted from the imaging system. Zip code was used as an alternative measure for socioeconomic status by extracting publicly available 2018 tax return data from the IRS’s website and stratifying into 6 range groups: <$25k, $25k-$50k, $50k-$75k, $75k-$100k, $100k-$200k, and $>200k. Ranges with over >20% AGI prevalence were selected as majority for a zip code, which could be assigned to one or multiple levels. Patients were stratified into three imaging groups: clinical trial, cost-recovery study, or commercial. For comparison, the racial makeup of prostate cancer patients at this single - institution were extracted from the institutional database.
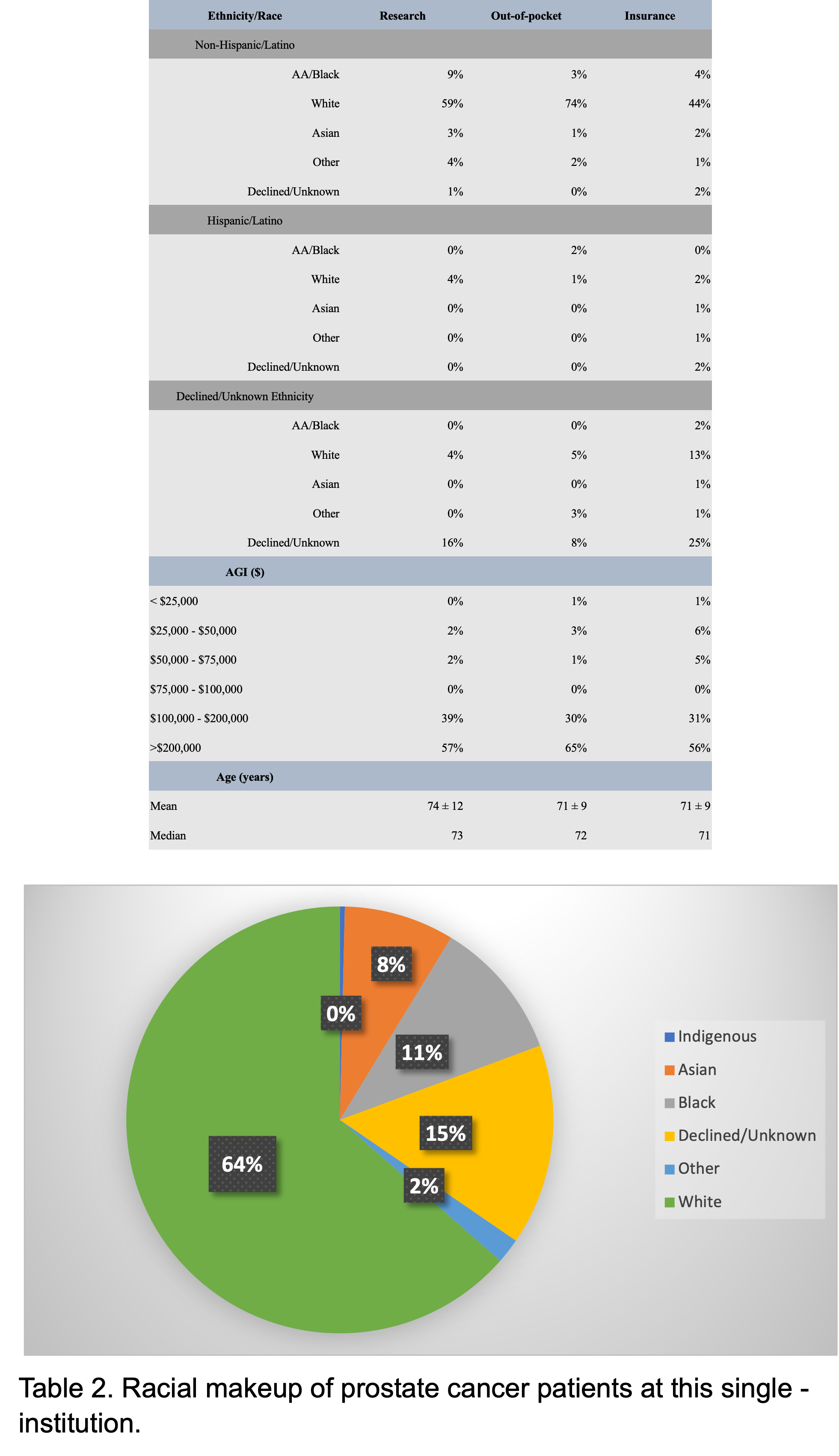
Results: 564 PSMA PETs were conducted. Table 1 compares the demographics and the AGI for each cohort. Almost double the number of African American (AA) patients were enrolled in the research cohort relative to the out-of-pocket and insurance cohort. Non-White Hispanic/Latino were the least likely to pay out of pocket for the scan. The institutional (n=1582) makeup of prostate cancer patients was predominantly non-Hispanic White (Table 2).
Conclusions: PSMA PET imaging was most commonly performed on white males (age > 70 year) at this single institution --findings consistent with similar institutions and nationwide PC biopsy data. AA patients were more likely to be scanned as participants in a clinical trial. Over 55% of the men in each cohort, however, resided in a zip code where over 20% of residents have an annual gross income over $200,000. This highlights that despite favorable insurance coverage, access is still limited by socioeconomic status, zip code and race.
Source of Funding: No funding
Methods: Patients with PC who underwent a PSMA PET scan between January 2018 and October 2021, were extracted from the imaging system. Zip code was used as an alternative measure for socioeconomic status by extracting publicly available 2018 tax return data from the IRS’s website and stratifying into 6 range groups: <$25k, $25k-$50k, $50k-$75k, $75k-$100k, $100k-$200k, and $>200k. Ranges with over >20% AGI prevalence were selected as majority for a zip code, which could be assigned to one or multiple levels. Patients were stratified into three imaging groups: clinical trial, cost-recovery study, or commercial. For comparison, the racial makeup of prostate cancer patients at this single - institution were extracted from the institutional database.
Results: 564 PSMA PETs were conducted. Table 1 compares the demographics and the AGI for each cohort. Almost double the number of African American (AA) patients were enrolled in the research cohort relative to the out-of-pocket and insurance cohort. Non-White Hispanic/Latino were the least likely to pay out of pocket for the scan. The institutional (n=1582) makeup of prostate cancer patients was predominantly non-Hispanic White (Table 2).
Conclusions: PSMA PET imaging was most commonly performed on white males (age > 70 year) at this single institution --findings consistent with similar institutions and nationwide PC biopsy data. AA patients were more likely to be scanned as participants in a clinical trial. Over 55% of the men in each cohort, however, resided in a zip code where over 20% of residents have an annual gross income over $200,000. This highlights that despite favorable insurance coverage, access is still limited by socioeconomic status, zip code and race.
Source of Funding: No funding


.jpg)
.jpg)